Rectocele and enterocele
What is a rectocele and an enterocele?
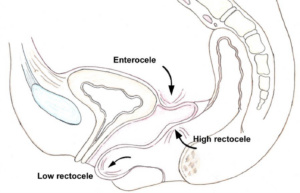
A rectocele is a bulge (hernia) that occurs in the front wall of the rectum and pushes it into the vagina. An enterocele is caused by the small bowel pushing into the vagina. These conditions occur mostly in women and it is thought that it may be a weak area in the female anatomy as the back wall of the vagina rests against the front wall of the rectum.
The risk of developing either a rectocele or an enterocele increase as a result of childbearing, particularly with problematic deliveries (for example long 2nd stage labour and/or the use of instruments to assist delivery), and multiple births. However, it is not unknown in younger women who have not had children and can also be associated with chronic constipation, straining to pass bowel motions, obesity, and hysterectomy.
Symptoms
Although rectoceles are fairly common, only a small proportion of people will have any symptoms. These can be felt through the vagina or the rectum. In the vagina a feeling of heaviness, painful intercourse and in some cases bleeding which may result from irritation. In certain cases, the hernia may protrude through the vaginal opening. In the rectum, symptoms can include increased need for straining in order to pass a stool and/or constipation a result of the bulge into the vagina effectively diverting material in the rectum away from the anus. Often a feeling of generalised pelvic pressure is reported.
Diagnosis
Diagnosis is usually made through a routine internal examination. An MRI scan or X ray may be used to determine the size and extent of the hernia.
Treatment
Treatment options vary depending on the degree of difficulty caused to the patient by the prolapse. Many women will have some form of mild prolapse without any symptoms, whilst for others the prolapse can protrude to a very great extent and affect toileting and intercourse as well as making the patient feel constantly uncomfortable.
In milder cases diet; ensuring that a good fibre and fluid intake reduces the need to strain to pass a motion and helps to avoid constipation, exercise; for example, pelvic floor exercises, pilates and yoga, to help strengthen the area and the use of pesaries, which help to support the vagina and are fitted on an individual basis, can all help with symptoms.
If the symptoms are causing issues with quality of life, surgery may be an option. This is most likely to be done through the vagina as the problems lies with the weakness of the supporting pelvic musculature. It will therefore be carried out by a gynaecological rather than a colorectal surgical team.
Outcomes and further sources of support
Because of inherent weakness, these problems can return following surgery and further procedures may be required. Adapting diet and lifestyle and maintaining a healthy weight does help with symptoms and can improve problems associated with going to the toilet.
Further information and support can be found at www.patient.info
